- Services
- Discovery & Intelligence Services
- Publication Support Services
- Sample Work

Publication Support Service
- Editing & Translation
-
Editing and Translation Services
- Sample Work

Editing and Translation Service
-
- Research Services
- Sample Work

Research Services
- Physician Writing
- Sample Work

Physician Writing Service
- Statistical Analyses
- Sample Work

Statistical Analyses
- Data Collection
- AI and ML Services
- Medical Writing
- Sample Work

Medical Writing
- Research Impact
- Sample Work

Research Impact
- Medical & Scientific Communication
- Medico Legal Services
- Educational Content
- Academic Editorial Services
- Educational Editorial Service
-
Education Editorial Services
-
- Industries
- Subjects
- About Us
- Academy
- Insights
- Contact Us
What Is Health Economy Research and How Does It Work?
- Home
- Academy
- Poster Presentation
- What Is Health Economy Research and How Does It Work?
Research Impact
- What Is Health Economy Research?
- Why Health Economy Research Matters in Healthcare
- How Does Health Economy Research Work?
- Methods Used in Health Economy Research
- How Health Outcomes Are Measured
- Role of Economic Modelling in Health Economy Research
- Real-World Applications of Health Economy Research
- Challenges and Limitations
- Future Directions in Health Economy Research
Interesting topics
What Is Health Economy Research and How Does It Work?
1. What Is Health Economy Research?
2. Why Health Economy Research Matters in Healthcare
3. How Does Health Economy Research Work?
4. Methods Used in Health Economy Research
5. How Health Outcomes Are Measured
6. Role of Economic Modelling in Health Economy Research
7. Real-World Applications of Health Economy Research
8. Challenges and Limitations
9. Future Directions in Health Economy Research
Health economics research analyses the allocation of scarce resources to maximize health outcomes, evaluating the efficiency, costs, and benefits of medical interventions and systems. It informs policy by studying healthcare financing, provider behaviour, and, increasingly, treating health as an investment for economic growth. Key areas include health behaviour, inequality, and measuring value using metrics like QALYs.[1] This integrated approach forms the foundation of Health Economics and Outcomes Research, linking costs, outcomes, and value generation across healthcare systems.
The growing demand on health systems worldwide is caused by rising costs, increasing age communities, and increasing medical invention. Health Economy Research is a critical area in meeting these demands, by reviewing how best to allocate limited healthcare resources to provide the highest health outcomes possible. It combines the principles of economics and real-world health data, facilitating evidence-based decision-making in policy, clinical care and Life Sciences. These activities collectively contribute to Outcomes Research in Healthcare by translating economic evidence into practical healthcare decisions.
1. What Is Health Economy Research?
Health Economics Research is a study of how health care resources are created, financed, distributed, and used in the best interests of the population in terms of health and the efficiency of the health care system. The Health Economics Research area will assess the financial implications, health outcomes, and value that result from a given activity (or intervention) in a health care system.[2,3] This scope is central to Health Economics Consulting Services that support healthcare payers, providers, and life sciences organizations. The Key focus areas include:
- Healthcare Financing and Reimbursement Mechanisms
- Economic evaluation of Pharmaceuticals, Devices, and Interventions
- Assessing Health Outcomes and Quality of Life
- Efficiency and Performance of Healthcare Delivery Systems
- Equity, Access, and Population Health Impact
THE INSIGHT:
Health economy research helps identify which healthcare interventions deliver the greatest health benefit relative to the resources invested.
2. Why Health Economy Research Matters in Healthcare
Healthcare has limited resources, but the need for healthcare continues to expand. The research in health economy provides decision-makers (purchasers & providers) with the important information they need to make justified, established and value-based decisions.[4] This evidence base is frequently used within Healthcare Market Access Strategy planning to support reimbursement and coverage decisions.
The significance of this research stems from the fact that it:
- Provides support for value-based health care decision making
- Provides information pertaining to pricing and reimbursement and coverage decisions
- Supports long-term financial viability of health care systems
- Identifies disparities in access to care and health outcomes. [5]
3. How Does Health Economy Research Work?
Research in health economics is a formalized, evidence-based procedure. The first stage involves characterizing an actual healthcare choice or decision-making issue in terms of whether a new intervention provides a benefit or value compared with alternative treatment options currently available. At this point, researchers will also determine which analytical perspective (health system, payer, or societal) will be used, and, using that perspective[6]. The data can be gathered from the following resources:
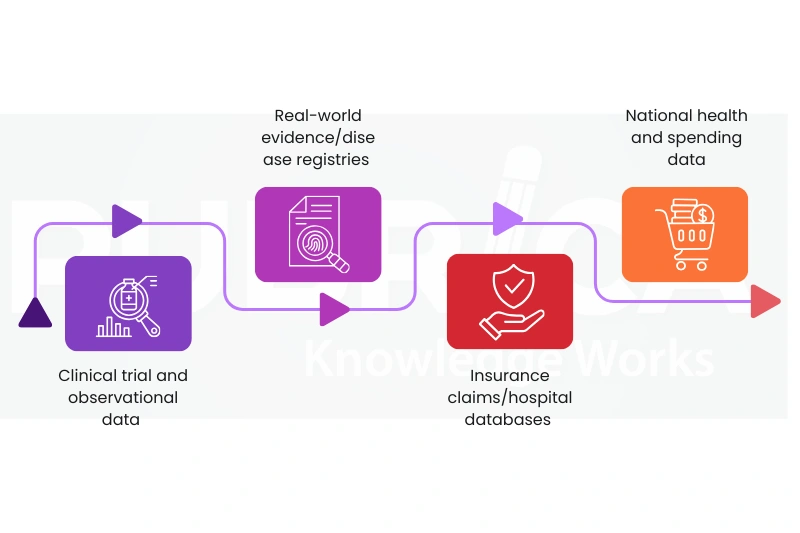
The structured use of Real-World Evidence in Health Economics strengthens the relevance of findings beyond controlled trial settings. This organized process assures that the results produced will sufficiently address both clinical effectiveness and economic viability.
4. Methods Used in Health Economy Research
To assess the value of an intervention, health economics research employs standardized economic evaluation techniques. The following types of are commonly used in the field of health economics:
| Method | What It Evaluates | Common Application |
| Cost-Effectiveness Analysis (CEA) | Cost per clinical outcome | Comparing treatment options |
| Cost-Utility Analysis (CUA) | Cost per QALY gained | Health technology assessment |
| Cost-Benefit Analysis (CBA) | Costs vs. monetary benefits | Public health programs |
| Budget Impact Analysis (BIA) | Affordability over time | Reimbursement planning |
The structured use of Real-World Evidence in Health Economics strengthens the relevance of findings beyond controlled trial settings.
5. How Health Outcomes Are Measured
Outcome measurement is central to health economy research. Outcomes capture not only survival but also quality of life and disease burden. Common Outcome Measures are listed below
Measure | Description |
Quality-Adjusted Life Years (QALYs) | Combines length and quality of life |
Disability-Adjusted Life Years (DALYs) | Measures total disease burden |
Health-Related Quality of Life (HRQoL) | Patient-reported quality of life |
Clinical Endpoints | Survival, symptom control, remission |
Example
When two treatments offer similar survival benefits, the intervention associated with better patient-reported quality of life at a lower cost is often preferred for reimbursement decisions
Quality Adjusted Life Years (QALYs) remain a standard metric used across Outcomes Research in Healthcare to compare interventions consistently.
6. Role of Economic Modelling in Health Economy Research
Long-term cost and outcome estimates can be obtained using economic models to evaluate long-term effects associated with treatment or disease progression beyond the time horizons of clinical trials. Economic models are commonly used to develop simulations of how diseases progress, paths of therapy, and levels of use of health care over long periods.[7] Common modelling approaches include:
- Decision tree models
- Markov models
- Microsimulation models
These modelling approaches are frequently delivered through Real World Evidence Analytics Services to support payer and policy decisions.
7. Real-World Applications of Health Economy Research
The analysis of health economics has a direct impact upon health decision making in many parts of the health system.
- Policy: Health technology assessment agencies employ cost-effectiveness thresholds to make decisions regarding coverage
- Industry: Pharmaceutical and medical device manufacturers utilise health economic evidence in their pricing and market access strategies
- Public Health: many vaccinations and prevention programmes are assessed by their long-term economic and population health effects.
8. Challenges and Limitations
Despite its value, health economy research faces challenges such as
- Not having adequate data types.
- Difficulties making long-term forecasts accurately; and
- Ethical dilemmas about how to classify the value of multiple different services
These applications directly inform Market Access and HEOR Strategy Services across life sciences organizations.
Credibility Check
Transparent assumptions, sensitivity analyses, and stakeholder engagement are essential to ensure that economic evidence remains trustworthy and policy-relevant
9. Future Directions in Health Economy Research
Due to the ongoing rapid advancement of the field, there is an increasing emphasis within this sector on the use of real-world evidence (RWE), digital health data, AI and value-based care models. In addition, there is a growing emphasis placed on using health equity and social determinants of health when conducting economic evaluations. These trends are shaping the evolution of HEOR Consulting Services globally.
Connect with us to explore how we can support you in maintaining academic integrity and enhancing the visibility of your research across the world!
Conclusion
Health Economics Research is a foundational element of today’s health care decision-making processes that enables decision-makers to better allocate limited resources in a more efficient and equitable manner through the systematic linking of cost with outcomes and value. Health Economics Research will remain an essential tool for supporting sustainable, patient-centred health delivery systems in times of financial and clinical pressure within the health care system. As demand grows, Health Economics Consulting Services will continue to play a critical role in supporting evidence-driven healthcare systems worldwide.
Ready to turn health economic evidence into impactful decisions? Partner with Pubrica to leverage robust Health Economics and Outcomes Research that supports market access, reimbursement, and value-based healthcare strategies. [Get Expert Publishing Support] or [Schedule a Free Consultation].
References
- Müller, M., & Petrisor, K. (2023, July 18). Health economics research. WifOR Institute. https://www.wifor.com/en/research
- Mcintyre, D., Meheus, F., & Røttingen, J.-A. (2017). What level of domestic government health expenditure should we aspire to for universal health coverage? Health Economics, Policy, and Law, 12(2), 125–137. https://doi.org/10.1017/S174413311600
- Neumann, P. J., Ganiats, T. G., Russell, L. B., Sanders, G. D., & Siegel, J. E. (Eds.). (2016). Cost-effectiveness in health and medicine(2nd ed.). Oxford University Press. https://doi.org/10.1093/acprof:oso/9780
- Porter, M. E. (2010). What is value in health care? The New England Journal of Medicine, 363(26), 2477–2481. https://doi.org/10.1056/NEJMp1011024
- Claxton, K., Martin, S., Soares, M., Rice, N., Spackman, E., Hinde, S., Devlin, N., Smith, P. C., & Sculpher, M. (2015). Methods for the estimation of the National Institute for Health and Care Excellence cost-effectiveness threshold. Health Technology Assessment (Winchester, England), 19(14), 1–503, v–vi. https://doi.org/10.3310/hta19140
- Weinstein, M. C., O’Brien, B., Hornberger, J., Jackson, J., Johannesson, M., McCabe, C., Luce, B. R., & ISPOR Task Force on Good Research Practices–Modeling Studies. (2003). Principles of good practice for decision analytic modeling in health-care evaluation: report of the ISPOR Task Force on Good Research Practices–Modeling Studies. Value in Health: The Journal of the International Society for Pharmacoeconomics and Outcomes Research, 6(1), 9–17. https://doi.org/10.1046/j.1524-4733.2003.00234.x
- Sonnenberg, F. A., & Beck, J. R. (1993). Markov models in medical decision making: a practical guide: A practical guide. Medical Decision Making: An International Journal of the Society for Medical Decision Making, 13(4), 322–338. https://doi.org/10.1177/0272989X93013