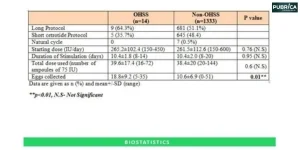
A Meta-Analysis of the Effects of Writing and Writing Instruction on Reading
January 6, 2022
A Systematic Assessment of the impacts of integrated healthcare in UK
January 17, 2022A Meta-Analysis of population studies on the prevalence of chronic pain in UK
Chronic pain, which includes illnesses like low back pain and osteoarthritis, was recently highlighted as one of the most common causes of disability worldwide by the Global Burden of Disease studies in a meta-analysis study. National governments have begun to acknowledge chronic pain as a key concern and challenge for their public health and healthcare systems, resulting in national plans and the convening of Pain Summits in countries such as the UK, US and Europe. As with other long-term conditions like cancer and cardiovascular disease, such initiatives emphasize the importance of accurate population-based estimates of chronic pain in helping to drive and inform policies of prevention and care, needs assessments, and surveillance of the impact of interventions. Despite multiple high-profile national publications emphasizing the importance of chronic pain in the UK, there is little agreement on the country’s pain burden. According to one estimate, up to 8 million people in the UK suffer from chronic pain, which corresponds to a telephone poll of European citizens in which 13% of the UK population reported pain of moderate-to-severe intensity that lasted for more than 6 months. Estimates based on definitions more closely aligned with those of the International Association for the Study of Pain: “pain that persists beyond normal tissue healing time, which is believed to be 3 months” was significantly higher than those cited in the European telephone survey. The goal of this clinical meta-analysis study was to compile available data on the prevalence of various chronic pain classifications in the general population to generate much-needed, reliable, and current national estimates.
Factors associated with chronic pain
Numerous physical, psychological, and social variables contribute to chronic pain. Risk factors have traditionally been categorized as “modifiable” or “non-modifiable,” however, this bio-medico-centric approach to epidemiology does not always account for the intricate interplay between modifiable and non-modifiable parts of each risk factor. For example, in meta-analysis studies, past experiences of violence or abuse are sometimes referred to as “non-modifiable” because the incident or events have already occurred, and the patient’s history cannot be altered. The individual’s explanation of these events and their impact on their life and health, on the other hand, is constantly changing, and this will affect their future health and life. In addition, interventions that strengthen the biopsychosocial determinants of health can help to prevent or reduce future population exposure to risk factors linked to chronic pain. Age, gender, ethnicity and cultural background, socioeconomic status, and lifestyle and behaviour are all considered factors. Identifying and managing modifiable risk factors and elements of risk factors may help avoid chronic pain or reduce its duration and severity. Meta analysis research factors that cannot be treated with medicine are relevant to discuss in a clinical setting. Many of these are pertinent to chronic pain predictions, evaluations, treatment, and prognoses, while others will be crucial in searching for new therapeutic targets. Chronic pain management requires a multidisciplinary, epidemiologically informed, and patient-centered approach.
The prevalence of chronic pain in the UK is estimated to be 43% based on the highest quality research of general population samples. Meta-analysis in research of chronic pain prevalence increases steadily with age, affecting up to 62% of the population over the age of 75, implying that the burden of chronic pain may rise even more as the population ages if the incidence remains unchanged. According to weighted averages, widespread chronic pain affects 14.2% of the population. Between 10.4% and 14.3% of the population suffers from either moderately or severely restricting chronic pain, resulting in an estimated 7.9 million persons in the UK with this condition.
Limitations
Given the meta-analysis heterogeneity in this field, which stems from differences in how chronic pain is characterized in each study and the populations analyzed, chronic pain epidemiology was chosen. The latter may impact the study’s generalizability to other people, regions, or countries. Differences in study design also limit individual research findings. Because of these distinctions, rigorous data synthesis, including meta-analysis, is complicated in this subject. Cross-sectional studies, in particular, make it challenging to demonstrate causation and, as a result, to separate risk factors from chronic pain outcomes.
Conclusions
Pubrica offers the best Clinical Meta-analysis services for clinical industries for younger researchers. We examine the best available statistics to show that chronic pain affects one-third to half of the population in the UK. Although prevalence data alone does not establish the need for care or prevention goals, reliable data on prevalence will aid public health, and healthcare officials prioritize this fundamental cause of distress and disability in the general population. Chronic pain’s enormous global illness burden must be addressed by addressing the causes and effects of chronic pain at both the individual and population levels. Modifiable risk factors (e.g. acute pain, lifestyle, and behaviour) must be addressed to avoid and lessen the burden of chronic pain, with the patient at the center of the care.
References
- A Fayaz1, P Croft2, R M Langford3, L J Donaldson4, G T Jones5; Prevalence of chronic pain in the UK: a systematic review and meta-analysis of population studies; Epidemiology Research; Volume 6 Issues 6.
- Sarah E.E. Mills, Karen P. Nicolson, Blair H. Smith; Chronic pain: a review of its epidemiology and associated factors in population-based studies; British Journal of Anesthesia; Volume 123, Issue 2, E273-E283, August 01, 2019.