Case Report on Healthcare Supply Chain Management
May 9, 2022
How to select Generic Medicines journals to submit the manuscript
May 24, 2022In brief
The Significant indirect evidence demonstrates that bipolar disorder (BIP) and major depressive disorder (MDD) are related (MDD). BIP and MDD have major depressive episodes in common; however, BIP is characterised by manic (bipolar 1) or hypomanic episodes in BIP (bipolar 2). Meta-Analysis Writing Services Considering overlap between genetic risk variables for both illnesses, genetic epidemiological and genome-wide linkage studies are also consistent to discover common genetic risk factors. To find common genetic risk factors, researchers conducted a survey. This blog reviews a meta-analysis combining data from genome-wide association studies by Liu and Youfang and coordinating with Blackwood (2009) for ascertainment and diagnostic assessment genotyping quality control and analysis.
Introduction
Recent research has challenged conventional diagnosis approaches that divide mood disorders into two distinct categories: bipolar and depressive disorders. The present taxonomy of mood disorders opposes Kraepelin’s concept of manic-depressive insanity as a single entity (illness). Recent study findings imply a relationship between bipolar disorders (particularly bipolar II disorder) and major depressive disorder. The following features currently point to a link between bipolar II disease and major depressive disorder:
Mixed depressive states (mixed depression) and dysphoric (mixed) hypomania (opposite polarity symptoms in the same episode do not support mood disorder splitting);
- Family history (major depressive disorder is the most common mood disorder in relatives of bipolar probands);
- Lack of points of equivalence between the depressive syndromes of bipolar II disorder and major depressive disorder;
- Bipolar major depressive illness with depression mixed states, early-onset age, atypical characteristics, bipolar family history, irritability, racing thoughts, and psychomotor agitation;
- A high proportion of major depressive disorders shift to bipolar disorders during long-term follow-up;
- A large proportion of people with serious depression have a history of manic or hypomanic symptoms;
- Factors of hypomania present in major depressive disorder episodes;
- The recurrent course of major depressive disorder; and
- Depressive symptoms are much more common than manic and hypomanic symptoms in the study of bipolar disorders.

Evidence Support Continuity Between Major Depressive Disorder and Bipolar Disorders
Bipolar disorder bipolar II is the most similar to major depressive disorder. As a result, Meta-Analysis Experts pursuing consistency focused on the connections between these two illnesses. There are some similarities between bipolar II illness and major depressive disorder.
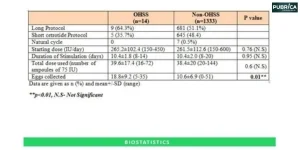
The procedures for determining, diagnosing, genotyping, quality control, and analysis are described elsewhere. Both investigations were carried out with the necessary ethical permissions, and all participants gave written informed consent. The majority of cases (81%) fulfilled DSM-IV (Diagnostic and Statistical Manual of Mental Disorders-IV) bipolar 1 criteria, with a lesser proportion (16%) fulfilling criteria for bipolar 2 (16%), schizoaffective disorder/manic type (2%), or bipolar NOS (not otherwise specified) criteria (1% ). Single nucleotide polymorphisms (SNPs) were evaluated after quality control (18.7% were genotyped directly, and the rest were imputed). Cases satisfying DSM-IV (Diagnostic and Statistical Manual of Mental Disorders-IV) criteria for MDD were found in clinical and community sources, while controls with low MDD risk were chosen from a population sample. Excessive missingness, uncommon genome-wide heterozygosity, and first- or second-generation mutations were all reasons for subjects being excluded.
Factors of hypomania in major depressive disorder
Depressive mixed states were seen in around 30% of individuals with major depressive illness. Apart from the raised mood factor, the factor structure of hypomania (outside depression) was comparable to that of depressed mixed states. In depressive diverse states (of major depressive disorder and bipolar II disorder), two hypomanic factors were found: the most common was a mental activation factor, which included racing and crowded thoughts and irritability, and the other was a motor activation factor, which included psychomotor agitation and more talkativeness. The occurrence of hypomania aspects inside the depression of major depressive disorder suggests that bipolar II disorder and major depressive disorder are associated.
It was found that depression and depressive symptoms were much more common than mania, hypomania, and manic and hypomanic symptoms in bipolar disorders (especially bipolar II disorder). This finding supports a link between bipolar disorders and major depressive disorder
Conclusion
CACNA1C risk polymorphisms may have a role in bipolar and unipolar major mood disorders, according to these Clinical Meta-Analysis Experts. According to certain theories, genetic variation in CACNA1C might be a frequent, modest, and pleomorphic risk factor for mental disorders. Alternatively, the overlap might be due to misclassification—for example, if some MDD patients were actually “bipolar-like” but were misclassified owing to diagnostic or nosological mistakes (despite using conventional and meticulous techniques), or if some BIP patients were similarly misclassified. The bipolar risk locus ANK3, on the other hand, received no support in this meta-analysis, indicating that its effect may be limited to BIP or that the power to detect an effect was low.
About Pubrica
Pubrica’s team of researchers and authors develop Scientific and medical research papers that can be indispensable tools to the practitioner/authors. Pubrica medical writers help you write and edit the introduction by introducing the reader to the shortcomings or empty spaces in the identified research field. Our experts know the structure that follows the broad topic, the problem, and background and advance to a narrow topic to state the hypothesis.
References
- Liu, Youfang, et al. “Meta-analysis of genome-wide association data of bipolar disorder and major depressive disorder.” Molecular Psychiatry 16.1 (2011): 2-4.
- Benazzi F. The relationship of major depressive disorder to bipolar disorder: continuous or discontinuous? Curr Psychiatry Rep. 2005 Dec;7(6):462-70. doi: 10.1007/s11920-005-0068-6. PMID: 16318825.